Clinical trials
Human challenge trials: pandemic exit strategy or ethical nightmare?
The UK is leading the way with implementing human challenge trials as a way to tackle the pandemic. Natalie Healey explores this unique study design, including the ethical and safety considerations and what it could teach us about the virus that causes Covid-19.
Should you deliberately expose someone to a deadly disease if it could eventually save many lives? That sounds like an ethical minefield and a violation of the Hippocratic Oath – but this method has a rich history in medical research.
Human challenge studies have helped scientists develop vaccines for many diseases such as cholera, typhoid and seasonal flu over the 20th and 21st centuries. The idea is that such trials fast-track the timeline for determining the safety and efficacy of a compound in development.
Clearly, this would be advantageous during the Covid-19 crisis when many uncertainties still abound about the virus that brought the world to a standstill. In February, the UK government announced it would run a Covid-19 human challenge study, following approval from the country’s clinical trials ethics body.
It is the first such study anywhere in the world for SARS-CoV-2. The initiative is a collaboration between Imperial College London, the Department for Business, Energy and Industrial Strategy, the Royal Free London NHS Foundation Trust and clinical trials company hVIVO.
The researchers hope the trial will ultimately help to reduce the spread of the coronavirus, mitigate its impact and reduce Covid-19 deaths.
After the ethics board gave the study the green light, the first part of the trial began at the Royal Free in early March. Healthy volunteers between the ages of 18 and 30 with no previous history of Covid-19 symptoms and no underlying health conditions or adverse risk factors for contracting severe disease with the coronavirus, such as diabetes, heart disease or obesity, signed up for the unusual trial.
On 25 March, the project team announced that the first three trial volunteers had completed a 14-day quarantine with no safety concerns and had since been discharged from the unit. The study will now progress to the next groups of healthy volunteers.
“We would like to thank these volunteers for their participation in this important study and look forward to welcoming the following cohorts,” said Andrew Catchpole, chief scientific officer at hVIVO, a subsidiary of contract research organisation Open Orphan, in a statement.
“We expect that this study will greatly assist our understanding of this disease and provide insights into its progression, natural immune response, and transmission.”
hVIVO has completed 50 human challenge studies since it was established in 1989. It says that over 3,000 volunteers have been inoculated using viruses such as flu, respiratory syncytial virus (RSV) and human rhinovirus.
In late March, the firm announced it had entered into a £7.5m contract with a US biotechnology company to run a human viral challenge study for an RSV prophylactic and treatment.
Ethics and safety
While many human challenge trials have led to important scientific advances, other studies have been highly controversial and a breach of human rights. For instance, in the 1940s in Guatemala, sex workers, prisoners and institutionalised patients were deliberately infected with syphilis and gonorrhoea without their knowledge and denied treatment.
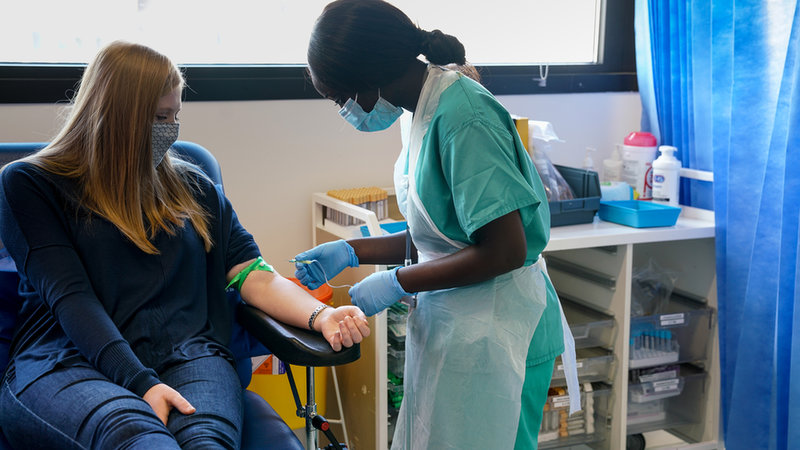
In the Covid trial, participants receive an initial health screening to check they are suitable for the study – including an antibody test to ensure they have not been previously infected by the coronavirus. Once volunteers are given the virus (in the form of a nasal spray), they will need to spend two weeks quarantining in hospital.
A medical team will closely monitor the volunteers for 14 days at a clinical facility. After they’ve left hospital, the volunteers will be called back regularly over the next 12 months for follow-up tests. They will be compensated around £4,500 over the course of a year.
But it is undeniably risky research, pointed out Joerg Hasford, president of the Association of Medical Ethics Committees in Germany in a letter in the British Medical Journal (BMJ) shortly after the trial was announced.
These studies should be treated as an opportunity to enhance and publicly demonstrate our highest moral standard.
At the time of writing, there are few effective treatment options for Covid-19 – certainly no sure-fire antidotes should someone get seriously ill following infection. It is for this reason, say the researchers, that volunteers are being recruited from groups that are statistically the least likely to develop severe illness when infected with the coronavirus.
hVIVO says it will maintain the Covid-19 trial volunteers’ anonymity until the study completes so cannot yet disclose further details of any results it has so far gathered. But some experts are calling for more transparency.
Writing in a blog for the BMJin March, Josh Morrison, executive director of 1Day Sooner, an advocacy group for research participants, and bioethicist Charles Weijer argue that the SARS-CoV-2 Human Challenge Programme researchers should publish the full study protocol.
“Evading public scrutiny is not a solution. Instead, these studies should be treated as an opportunity to enhance and publicly demonstrate our highest moral standards,” they write.

Knowledge gains
Some may wonder whether human challenge studies are needed at all given that several safe and effective Covid-19 vaccines are already available.
Proponents say that this type of trial will uncover findings that are impossible to elucidate from real-world data, such as how much coronavirus is needed to trigger infection and why certain people experience moderate to severe disease with Covid-19 and others have no symptoms at all.
Another argument for human challenge studies is vaccination isn’t a fail-proof way out of the pandemic. New variants that may evade immunity gained naturally or through inoculation could undermine a country’s vaccination programme.
In human challenge studies, researchers will also be able to test if new generations of vaccines are effective against such new strains of the coronavirus. And, as the prevalence of Covid-19 varies in populations – and will likely continue to fall as more countries roll out their vaccination programmes – it is difficult for traditional vaccine trials to determine whether the jabs are effective if fewer people are naturally exposed to it.
Data from this study will provide key insights into how Covid-19 affects us.
Human challenge trials would enable researchers to continue studying the coronavirus even when prevalence in the community is very low, giving us a head start should infection rates increase again.
“Not only can human infection studies speed up vaccine development, but data from this study will provide key insights into how Covid-19 affects us from as soon as we are infected, which will potentially inform research into new treatments,” said Charlie Weller, head of vaccines at Wellcome, in a Science Media Centre statement.
“Together, effective treatments, vaccines and testing will help communities around the world to protect themselves and bring this pandemic to an end.”